

Views: 0 Author: Site Editor Publish Time: 2026-03-24 Origin: Site











Missing a tooth affects more than your smile. It can change how you chew and speak.An Implanting Crown helps replace the visible tooth. It also works with the implant below the gum.In this article, you will learn what it is. You will also see how it works and why it matters.
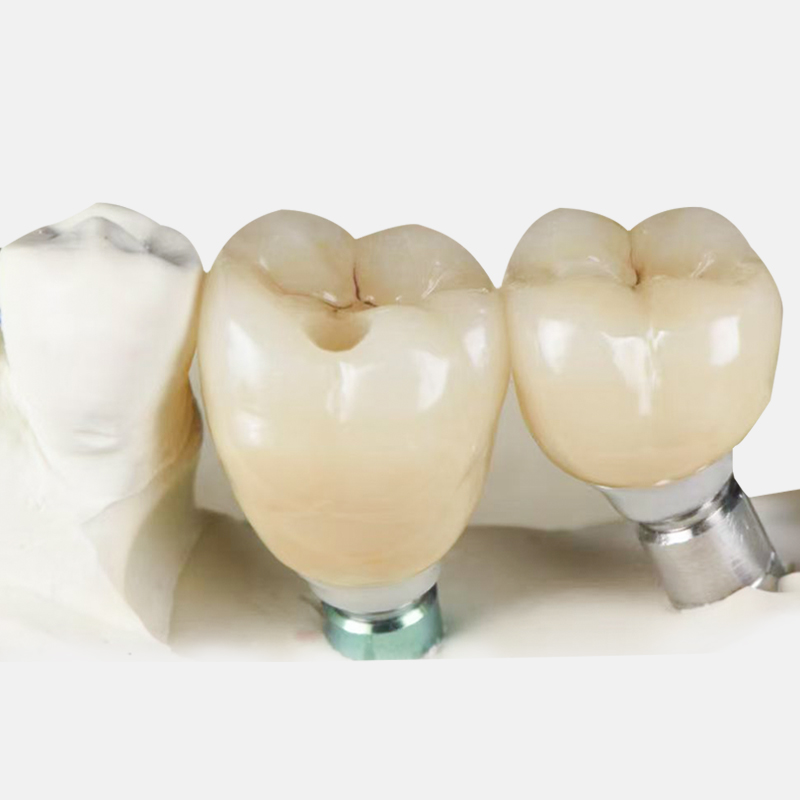
An Implanting Crown is the visible prosthetic tooth attached to a dental implant system, and its job is to restore the part of the tooth that extends above the gumline, allowing the patient to chew, speak, and smile with improved comfort and confidence. Unlike a traditional crown, which covers and protects a damaged natural tooth that still has a root and some remaining structure, an Implanting Crown is used when the natural tooth is already missing, so it does not cap an existing tooth but instead becomes the visible top portion of a replacement tooth system.
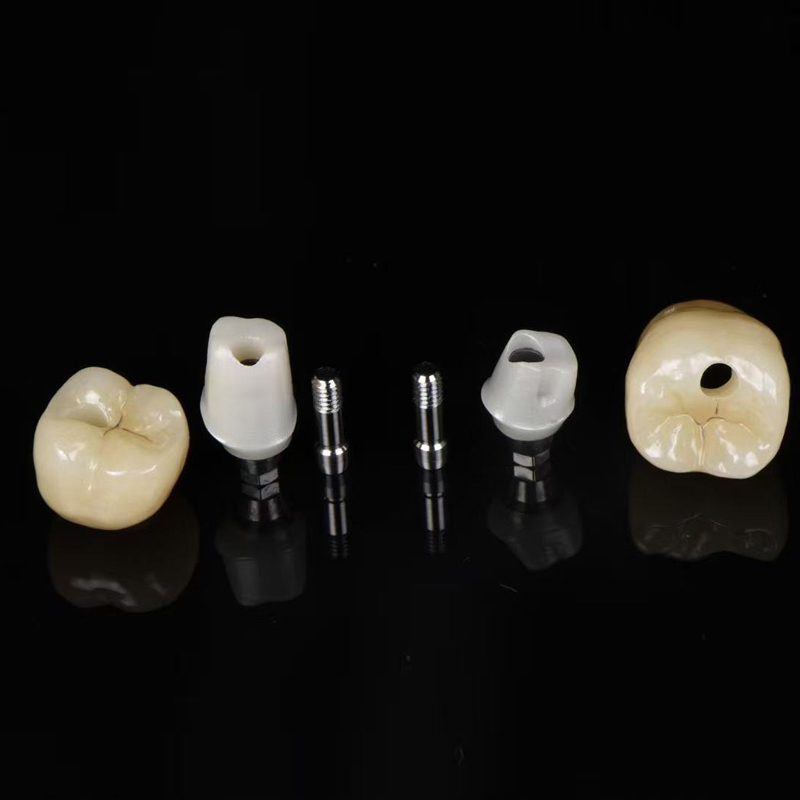
To understand this clearly, it helps to look at the three-part structure of the restoration, because many patients and even some non-specialist buyers tend to focus only on the crown itself and forget that its success depends on the foundation beneath it. The implant fixture is placed inside the alveolar bone and acts like an artificial root, the abutment sits above the implant and creates the connection point, and the crown is then secured on top to recreate the visible tooth form, which means the final clinical result depends on the precision of all three parts rather than the crown alone.
This distinction is more than academic, because it affects expectations about treatment time, cost, maintenance, and function. A regular crown can often be completed faster because it builds on a tooth that is still present, whereas an Implanting Crown usually requires a staged treatment process involving implant placement, healing, and final restoration, which is slower but often provides more independent support because it does not rely on neighboring teeth for retention. For patients who want a tooth replacement that feels rooted rather than removable, this difference is often one of the strongest reasons to consider an implant-supported solution.
The way an Implanting Crown works becomes much easier to understand when we stop thinking of it as a single product and instead see it as the visible endpoint of a biologic and mechanical system, because the final crown only performs well when the implant beneath it has integrated with the surrounding bone and the connection between the internal and external parts is stable. In most cases, the implant, which is often made of titanium or another biocompatible material, is placed surgically into the jawbone, and over time the bone heals tightly around its surface in a process called osseointegration, which gives the implant the stability needed to support the final crown during chewing and daily use.
Once the implant has integrated successfully, the clinician attaches an abutment, which is the connector between the implant platform and the visible crown, and this small component plays a much larger role than many readers realize because it affects crown angulation, emergence profile, soft tissue support, and the fit of the final restoration. After that, the Implanting Crown is designed and fabricated so it can be attached to the abutment or directly to the implant interface, depending on the restorative system and attachment method chosen for the case. When planned properly, the finished restoration restores not only appearance but also functional tasks such as biting, chewing, speaking clearly, and maintaining proper contact with neighboring and opposing teeth.
The reason implant-supported crowns are often described as feeling more stable than removable alternatives is that their support comes from within the bone rather than from the gum alone or from adjacent teeth, so they are structurally different from dentures and mechanically different from conventional bridges. A denture rests on soft tissue and can shift during function, while a bridge depends on neighboring teeth that may need preparation, but an Implanting Crown stands on its own implant base, which allows it to distribute force in a way that more closely resembles a natural tooth. That does not mean every implant crown feels identical to a natural tooth, but it does explain why many patients report improved chewing confidence and better day-to-day comfort after successful treatment.
The natural appearance of an Implanting Crown depends just as much on restorative design as on the implant itself, because the crown must be shaped and shaded to blend with surrounding teeth and to support the contour of the soft tissue around it. Digital scanning, CAD design, and precision milling have made this part of the workflow much more accurate, allowing labs to refine contacts, margins, translucency, and occlusion more consistently than in older manual workflows. This is also where high-quality manufacturing partners become important, because a crown that looks good in theory must still be milled, sintered, finished, and inspected accurately if the final result is meant to be clinically reliable and commercially valuable.
The treatment sequence for an Implanting Crown usually unfolds over several stages, and understanding these stages helps readers appreciate why implant dentistry often takes longer than bridge treatment or removable prosthetic replacement, even though the final result may offer better independence and support. The first phase is consultation and treatment planning, during which the dentist evaluates oral health, gum condition, bite relationship, medical history, and available bone volume, often using radiographs or three-dimensional imaging to determine whether implant placement is feasible and whether additional procedures such as extraction, grafting, or soft tissue management may be needed.
If the site is ready, the implant is placed surgically into the bone, but if the patient still has a failing tooth or insufficient bone in the area, there may be preliminary steps before that, such as extraction or bone augmentation, and these extra procedures can extend the timeline while improving the stability and esthetic potential of the final restoration. After implant placement, the healing phase begins, and this period is not merely passive waiting, because the implant must achieve biologic integration with the bone before the restoration can carry normal functional loads. Depending on the case, healing may take several months, and while immediate provisional restorations are possible in selected situations, the final crown is usually delayed until the supporting tissues are stable.
Once healing has progressed sufficiently, the restorative phase begins, which generally includes abutment selection, impression taking or digital scanning, and design of the final crown. At this point, both the clinician and the lab focus on precise margin adaptation, occlusal harmony, contact points, esthetic integration, and the relationship between the crown and the soft tissue. A high-quality Implanting Crown should not only seat accurately but also support an emergence profile that looks natural and is easy for the patient to keep clean. This is why the restorative phase is not simply about placing a tooth-shaped object on top of an implant, but about translating clinical planning into a durable, functional, and biologically compatible final result.
For dental labs and procurement teams, the clinical timeline also intersects with workflow expectations, because the lab’s production speed, file compatibility, material handling, and communication quality all affect how smoothly a case moves from scan to delivery. In the product information you provided, Shenzhen Lezy Jumei Dental Medical Co states that it supports OEM and ODM manufacturing for dental labs, accepts digital case files such as STL, PLY, and DCM, and typically completes production in about three days before shipping, which reflects the growing role of digital manufacturing partners in modern implant restorative workflows. When such turnaround claims are paired with strong quality control and good case communication, they can help labs reduce delays and maintain more predictable schedules.
Although patients often think of the crown as a single final piece, the way an Implanting Crown attaches to the implant is an important clinical and technical decision because it influences esthetics, retrievability, maintenance, and the way future complications are managed. The two most common attachment methods are screw retention and cement retention, and both approaches are widely used in implant dentistry, though each has strengths that make it more suitable in certain clinical scenarios rather than universally better in all cases.
A screw-retained Implanting Crown is secured with a small screw that passes through the restoration or its framework into the implant or abutment, and one of its main advantages is retrievability, because the clinician can often remove the crown later for repair, maintenance, or inspection without destroying it. This is especially useful in complex cases, posterior restorations, and multi-unit implant-supported prostheses where long-term access matters. The trade-off is that the screw access opening may affect esthetics or occlusion if implant angulation is not ideal, though modern planning and restorative materials can often manage that limitation effectively.
A cement-retained Implanting Crown, by contrast, is fixed in place using dental cement, which can create a cleaner visible surface because there is no access hole on the crown surface, making it attractive for some anterior or highly esthetic cases. However, the lack of easy retrievability can become a disadvantage later if the crown needs to be removed, and excess cement, if not managed carefully, may also contribute to peri-implant soft tissue problems. This is why the choice between the two methods should be driven by implant angle, esthetic priority, tissue conditions, occlusal needs, and long-term maintenance planning rather than by appearance alone.
Attachment Method | Key Advantage | Main Limitation | Best-Fit Situations |
Screw-Retained Implanting Crown | Easier retrieval for repair, inspection, and maintenance | Access hole may influence esthetics or occlusion | Posterior crowns, full-arch bridges, maintenance-focused cases |
Cement-Retained Implanting Crown | Smooth external appearance and simplified visible contour | Harder to remove later and technique-sensitive cement control | Anterior zones, selected high-esthetic cases |
Hybrid or Advanced Restorative Designs | Can combine structural and functional advantages in complex cases | Higher design and fabrication complexity | Full-arch restorations, screw-retained hybrid prosthetics, implant bridges |
The product information you shared also shows that the Implanting Crown category extends beyond single-unit crowns into broader implant restorative solutions such as full-arch zirconia implant bridges, screw-retained hybrid prosthetics, and custom implant-supported crowns and bridges, which is important for B2B readers because it frames the product not as a narrow item but as part of a scalable restorative portfolio. When a manufacturer can support both standard and advanced designs across major implant systems, it becomes more relevant for labs that want to handle a range of implant cases rather than outsourcing difficult restorations elsewhere.
Material selection is one of the most important decisions in the design of an Implanting Crown, because the restoration must balance strength, translucency, wear behavior, milling accuracy, and long-term esthetic performance rather than excelling in only one category. In visible anterior cases, esthetics often receives more attention because color integration and light transmission strongly affect how natural the restoration appears, while in posterior cases, resistance to fracture and functional durability often take priority because bite loads are heavier and restorative failure can become more costly for both clinic and lab.
Porcelain-based ceramics are often valued for their ability to reproduce enamel-like optical properties, which is why they remain attractive when the visible appearance of the restoration is the primary concern. Zirconia, however, has become one of the most important materials in implant crown manufacturing because it combines high strength with increasingly improved translucency, allowing it to serve both functional and esthetic demands more effectively than older generations of opaque ceramics. According to the product data you provided, the Implanting Crown line from Shenzhen Lezy Jumei Dental Medical Co uses high-purity medical-grade zirconia and offers flexural strength ranging from 600 MPa to 1350 MPa, which indicates that the material portfolio is designed to serve both lower-load and higher-load restorative needs.
The same specification sheet lists translucency levels of 40% to 59%, availability in VITA 16 Classic Shades and bleach shades BL1 to BL4, and compatibility with major digital manufacturing systems including Open System 98 mm, Zirkonzahn 95 mm, and Amann Girrbach 92 mm, which is commercially significant because material performance alone is not enough if the product does not integrate well into the lab’s existing equipment and workflow. In implant restorative manufacturing, material choice and system compatibility are deeply connected, since the wrong combination can create inefficiency, higher remake rates, or inconsistent sintering results.
Porcelain-fused-to-metal restorations still retain value in some workflows because they offer a familiar balance of structural support and acceptable esthetics, but many labs increasingly prefer high-quality zirconia for implant crowns because it supports more streamlined digital production and often reduces concerns about chipping when the case is designed and processed correctly. The recommended sintering range in your product data, 1450°C to 1530°C depending on product type, further highlights the fact that zirconia restorations are not simply milled and delivered, but must be processed within controlled manufacturing parameters to achieve the intended strength and esthetic outcome.
Material / Option | Main Benefit | Typical Clinical or Lab Value | Notes from Product Data |
High-Purity Medical-Grade Zirconia | High strength plus good esthetics | Suitable for single crowns, bridges, and implant restorations | Flexural strength 600–1350 MPa; translucency 40%–59% |
Porcelain | Excellent natural optical effect | Useful in highly esthetic zones | Often selected when appearance leads the case |
Porcelain-Fused-to-Metal | Balanced strength and familiarity | Practical in certain conventional workflows | May offer lower translucency than advanced ceramics |
Titanium / Co-Cr Framework Options | Strong substructure support | Useful in frameworks and reinforced designs | Listed as available framework options |
Multi-Layer Zirconia Series | Better shade and translucency transition | Supports more lifelike anterior or mixed esthetic cases | Supports natural gradient effect in final crown design |
The value of an Implanting Crown lies in the way it combines restorative independence, functional support, and esthetic integration, making it attractive not only to patients seeking a natural-looking result but also to clinicians and labs who want a solution that can perform consistently over time. Because the crown is supported by an implant rather than by neighboring teeth, it can restore a missing tooth without requiring preparation of adjacent healthy teeth, which is one of the clearest structural advantages over some bridge-based alternatives. This makes it especially appealing in cases where surrounding teeth are intact and preserving them is part of the treatment goal.
Another major benefit is improved chewing stability, because implant-supported restorations usually feel firmer than removable options and often allow patients to bite with greater confidence once healing is complete and the restoration is properly adjusted. That functional improvement often has an emotional side as well, since patients who regain comfortable chewing and a natural smile tend to report better confidence in both social and professional settings. Still, responsible content should avoid oversimplified promises, because results vary depending on bone quality, tissue health, bite patterns, and long-term maintenance habits.
From a biologic standpoint, implants also help provide stimulation to the jawbone in the area of the missing tooth, which may help reduce the bone loss that often follows tooth extraction. While the Implanting Crown itself is the visible component, its value is linked to the implant beneath it, because together they restore both support and contour in a way that more closely resembles a natural tooth than many non-implant alternatives. For clinicians and labs, the benefit is not merely cosmetic, but also structural and long-term.
For B2B readers, the advantages also include digital efficiency, material consistency, and fewer remakes when high-grade zirconia and well-controlled CAD/CAM production are used. The product profile you shared emphasizes exceptional strength, multilayer esthetics, compatibility with major systems, and digital manufacturing precision, while also noting certifications such as FDA, CE, and ISO 13485, which are highly relevant in supplier evaluation because they help build confidence in product traceability, regulatory alignment, and manufacturing discipline. When a lab selects a supplier for Implanting Crown production, it is often making a decision not only about materials but also about reliability, communication, warranty support, and the ability to handle both routine and complex cases.
A well-designed Implanting Crown can be an excellent solution, but it is not automatically the right option for every patient at every moment, which is why careful case selection remains central to responsible treatment planning. In general, good candidates have healthy or treatable gums, adequate bone support or the ability to receive bone augmentation if needed, stable medical conditions, and a realistic understanding of the treatment timeline and maintenance requirements. The presence of good oral hygiene habits is especially important, because even the strongest restorative materials cannot compensate for chronic plaque accumulation or neglected soft tissue inflammation around implants.
Bone quality and quantity matter because the implant must achieve stable support in the jaw, and if the bone is severely reduced, grafting or site development may be required before predictable restoration becomes possible. Certain habits and conditions also deserve closer attention, including smoking, uncontrolled diabetes, heavy bruxism, and complex occlusal patterns, since they can affect healing, implant loading, and long-term restorative wear. This does not mean patients with these conditions are always excluded, but it does mean that treatment planning should be individualized rather than based on generic promises.
For labs and implant restoration suppliers, understanding candidacy also has practical value because it shapes case expectations and communication. A precisely manufactured Implanting Crown cannot solve problems created by unstable tissue, incorrect implant position, or unresolved parafunctional loading, so technical excellence must always be matched by sound clinical planning. Strong articles acknowledge this reality, because trustworthy content helps readers understand not only who may benefit most from the restoration, but also why some cases require additional preparation or caution before the final crown is ever made.
The lifespan of an Implanting Crown depends on far more than the crown material alone, because long-term success is influenced by bite force, hygiene, implant positioning, occlusal adjustment, soft tissue health, and the quality of ongoing maintenance after placement. In many cases, the implant itself can remain stable for a very long time when the surrounding bone and tissue stay healthy, while the crown, which absorbs daily functional wear, may need replacement earlier if it chips, loosens, wears down, or becomes esthetically outdated. That is why it is more accurate to think of the implant as the long-term foundation and the crown as the visible component that may require future service even when the implant remains successful.
Daily care for an Implanting Crown should be explained in practical rather than dramatic terms, because the habits involved are familiar but important: patients should brush thoroughly, clean between teeth and around the implant area, maintain the gumline carefully, and attend regular professional checkups so that small problems can be identified before they become costly complications. Poor hygiene, missed recalls, heavy grinding, and the habit of chewing hard objects can all shorten the useful life of the restoration, and symptoms such as looseness, pain on biting, bleeding around the implant, gum swelling, or visible chipping should prompt timely professional evaluation rather than delay.
For B2B buyers, aftercare and warranty support are part of the product story because restorative success does not end at shipment. The information you provided states that Shenzhen Lezy Jumei Dental Medical Co offers up to a 3-year manufacturer’s warranty on fixed restorations and 1 year on removable prosthetics, while also providing online technical support through channels such as phone, video, or WhatsApp, which strengthens the brand’s value proposition for labs that want dependable case follow-up in addition to manufacturing capability. In a competitive dental supply environment, this type of support can be as important as raw material strength because it reduces procurement risk and improves trust.
An Implanting Crown restores the visible part of a missing tooth. It works with the implant and abutment to rebuild function and appearance.Its success depends on fit, material choice, and daily care. A well-made restoration can improve chewing, comfort, and smile confidence.Shenzhen Lezy Jumei Dental Medical Co., Ltd. adds value through precise CAD/CAM zirconia restorations, certified quality, and OEM/ODM support.
A: An Implanting Crown is the visible tooth attached to a dental implant.
A: An Implanting Crown connects to an abutment and restores chewing, speech, and appearance.
A: It stands independently, helps support bone, and avoids cutting nearby teeth.
A: Cost varies by case and material, and it can last many years with proper care.